Warfarin-Antibiotic Interaction Checker
Please select an antibiotic from the dropdown menu to see the potential interaction with Warfarin.
Taking an antibiotic while on a blood thinner can feel like a routine part of getting healthy, but for people using Warfarin is a vitamin K antagonist anticoagulant used to prevent blood clots, it's a high-stakes combination. The problem isn't the antibiotic itself, but how it changes the way your body processes the medication. If the balance shifts, your blood can become too thin, leading to dangerous INR spikes and a significant increase in bleeding risk.
Quick Summary: Key Takeaways
- Most antibiotics increase the effect of Warfarin, which can raise your INR and increase bleeding risk.
- Interactions happen either by blocking liver enzymes (CYP2C9) or killing vitamin K-producing bacteria in your gut.
- High-risk drugs include Ciprofloxacin, Bactrim, and certain Macrolides.
- INR monitoring is essential within 72 hours of starting or stopping an antibiotic.
- Rifampin is a rare exception that actually lowers INR, increasing the risk of clots.
Why Antibiotics Mess With Your INR
To understand why this happens, you first have to know what the INR (International Normalized Ratio) is. It's a standardized measurement of how long it takes your blood to clot. For most people on Warfarin, the target range is between 2.0 and 3.0. If that number climbs above 4.0, the risk of a major bleed increases by four to eight times.
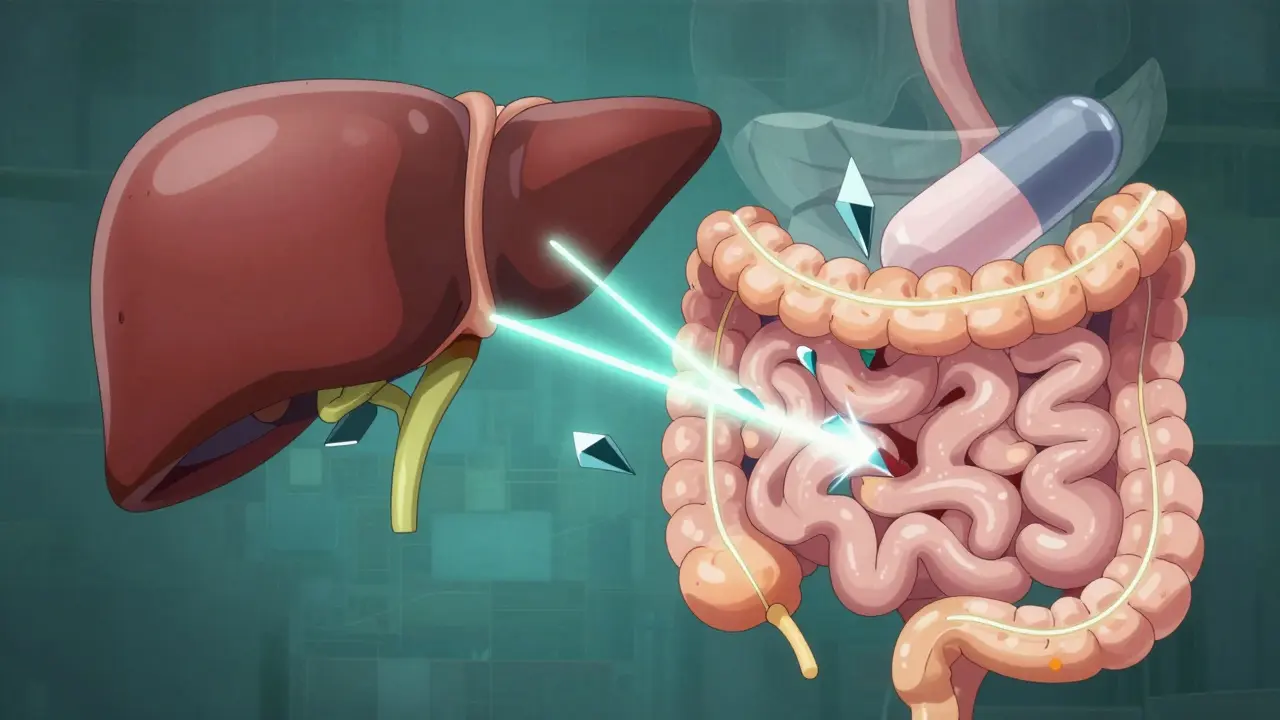
Antibiotics throw this balance off in two main ways. First, some drugs block the CYP2C9 enzyme in your liver. Since this enzyme is responsible for breaking down the most potent part of Warfarin, blocking it means the drug stays in your system longer, making your blood thinner. Second, antibiotics kill the bacteria in your gut. While we usually think of gut bacteria as just for digestion, some of them actually produce vitamin K. Because Warfarin works by blocking vitamin K, having less of it in your system makes the drug feel even stronger.
The High-Risk Antibiotics You Should Watch
Not all antibiotics are created equal when it comes to bleeding risks. Some are relatively quiet, while others can cause your INR to skyrocket in just a few days. Fluoroquinolones, like Ciprofloxacin, are particularly aggressive. In some clinical observations, patients saw their INR jump from a stable 2.5 to a dangerous 4.1 within a single week of starting the medication.
Then you have Sulfamethoxazole/Trimethoprim (commonly known as Bactrim). This combination is notorious for elevating INR levels quickly, often by nearly two full units within five days. Macrolides like Erythromycin also pose a high risk because they strongly inhibit liver enzymes, whereas Azithromycin is generally gentler on the system.
It's also worth noting that some antibiotics, like Amoxicillin/Clavulanate, don't interfere with liver enzymes at all. Instead, they work purely by wiping out your gut flora, which means the INR spike might happen a bit slower-usually 5 to 7 days after you start the pills.
| Antibiotic Class | Example Drug | Effect on INR | Primary Mechanism |
|---|---|---|---|
| Fluoroquinolones | Ciprofloxacin | Significant Increase | CYP2C9 Inhibition |
| Sulfonamides | Bactrim | Significant Increase | CYP2C9 Inhibition |
| Macrolides | Erythromycin | Moderate to High Increase | CYP3A4/CYP2C9 Inhibition |
| Penicillins | Amoxicillin | Moderate Increase | Gut Flora Depletion |
| Rifamycins | Rifampin | Significant Decrease | Enzyme Induction |
The Danger of Rifampin: A Different Story
While most antibiotics make you bleed more, Rifampin does the exact opposite. It is a potent enzyme inducer, meaning it tells your liver to work overtime and chew through Warfarin much faster than usual. This can drop your INR below 1.5, which puts you in a "hypercoagulable" state-basically, your blood is too thick, and you're at a higher risk for a stroke or a deep vein thrombosis.
Because of this, Rifampin often requires a massive dose increase of Warfarin-sometimes 50% to 100% more-just to keep the INR in the safe zone. It's a complete 180 from the risks associated with Ciprofloxacin or Bactrim, which is why your doctor needs to know exactly which antibiotic you're taking.
How to Manage the Risk Without Panicking
You don't have to avoid antibiotics, but you do need a plan. The gold standard for management is a "test early and test often" approach. According to the American College of Chest Physicians, you should have your INR checked within 72 hours of starting an antibiotic. This allows your doctor to catch a spike before it becomes a medical emergency.
Depending on the drug, your healthcare provider might suggest a preemptive dose reduction. For high-risk CYP inhibitors (like fluoroquinolones), some clinics recommend cutting your Warfarin dose by 20-30% immediately upon starting the antibiotic. For others, like cephalosporins, the strategy is usually just to monitor weekly and only adjust the dose if the INR actually starts to climb.
Keep in mind that the risk doesn't disappear the moment you swallow your last pill. While liver enzyme effects usually resolve within 72 hours of stopping the drug, the gut flora effect can linger. Your vitamin K-producing bacteria take time to grow back, meaning your INR could stay unstable for 7 to 10 days after the antibiotic course is finished.
Spotting the Warning Signs
Numbers on a lab report are one thing, but you need to know what's happening in your own body. When your INR is too high, your blood cannot clot efficiently. You should contact your anticoagulation clinic immediately if you notice any of the following:
- Unusual or easy bruising (bruises appearing without a known bump or fall).
- Blood in your urine (which may look pink or red) or stool (which may look black and tarry).
- A nosebleed that won't stop after 10 minutes of pressure.
- Gums that bleed excessively when you brush your teeth.
- Small red or purple spots on your skin (petechiae).

Looking Ahead: Personalized Medicine
The future of managing these interactions is getting much more precise. Doctors are starting to look at pharmacogenetics-the study of how your genes affect your response to drugs. For example, people with specific variants of the CYP2C9 gene (specifically the *2 and *3 variants) are’ve been found to experience INR increases that are 2.4 times higher than average when taking antibiotics.
New trials, like the WARF-GEN study, have shown that using your genetic profile to guide dosing can reduce INR instability by over 40%. Instead of a one-size-fits-all dose reduction, we're moving toward a world where your a doctor knows exactly how you'll react to a specific antibiotic before you even take the first dose.
Which antibiotics are safest for people on Warfarin?
While no drug is entirely without risk, Nitrofurantoin and Fosfomycin are generally considered to have minimal interaction with Warfarin. Newer antibiotics like Tedizolid also show very little effect on INR levels. However, any new medication should still be reported to your healthcare provider.
How quickly can an antibiotic cause an INR spike?
It depends on the mechanism. Drugs that inhibit liver enzymes (like Ciprofloxacin or Bactrim) can cause an increase within 48 to 72 hours. Drugs that affect gut bacteria (like Amoxicillin) typically take longer, with the effect manifesting 5 to 7 days after you start the treatment.
Should I stop taking my antibiotic if my INR goes up?
No, never stop an antibiotic without talking to your doctor, as this can lead to antibiotic resistance or a return of the infection. Instead, your doctor will likely adjust your Warfarin dose (reducing it) to bring your INR back into the target range while you finish your course of antibiotics.
Why does my doctor want to check my INR after I finish the antibiotics?
Because some antibiotics kill gut bacteria that produce vitamin K, your body needs time to recover those bacteria. This means your INR can remain unstable for 7 to 10 days after the medication is gone. Testing after the course ensures you don't need to increase your Warfarin dose back to its original level too quickly or too slowly.
Can I take a probiotic to prevent INR spikes?
While probiotics are often used to restore gut health, they are not a substitute for INR monitoring. There is no clinical evidence that a standard probiotic can reliably prevent the CYP2C9 inhibition caused by drugs like Bactrim or Ciprofloxacin. Always rely on blood tests to manage your dosing.
Next Steps and Troubleshooting
If you've just been prescribed an antibiotic, the first thing you should do is notify your anticoagulation clinic. Don't wait for your next scheduled appointment. Ask your provider if a preemptive dose reduction is necessary based on the specific antibiotic class you're receiving.
For those who find their INR is consistently unstable during illness, it's worth asking your doctor about a "sick day protocol." This is a pre-approved set of instructions on how to adjust your dose and when to test your blood during an infection. If you have a family history of drug sensitivity, you might also discuss genetic testing for CYP2C9 variants to help predict your future reactions.






Quinton Bangerter
April 20, 2026 AT 05:52Of course they want you to get genetic testing now. Just another way for big pharma to harvest your DNA and put you in a database while they push these "personalized" doses that probably just make the drugs more addictive or controllable. The whole INR system is basically a guessing game anyway and they know it.
Shalika Jain
April 20, 2026 AT 22:05Imagine actually believing that a generic a-la carte list of antibiotics is enough to keep you safe. Please. The nuance here is completely missing if you think a simple table is the peak of medical advice. It's almost quaint how simplified this is.
Valorie Darling
April 21, 2026 AT 11:09idk why everyone is stressing just call the doctor and chill lol
Bob Collins
April 22, 2026 AT 08:26It's quite a lot to manage, but sticking to the 72-hour window for testing is a solid bit of advice for anyone feeling overwhelmed by the process.
anne camba
April 23, 2026 AT 02:43The fragile balance of our internal chemistry is a mirror to the instability of the human condition... it is truly fascinating how a tiny pill can disrupt the very rhythm of our blood's flow!!!
Don Drapper
April 24, 2026 AT 15:36The presentation of this data is laughably inadequate. To suggest that a 20-30% dose reduction is a universal "recommendation" without providing the precise pharmacokinetic curves for each drug class is an absolute travesty of clinical analysis! It is an affront to actual science!
dallia alaba
April 25, 2026 AT 08:03For those who are new to anticoagulants, please remember that diet also plays a massive role here, especially with vitamin K intake. If you're starting an antibiotic that wipes out gut bacteria, you might find your reaction to leafy greens becomes more volatile than usual. It is all about that synergy between the medication, the gut microbiome, and your dietary habits. I've seen many patients struggle because they only focused on the drug interaction and forgot that their spinach salad suddenly had a different impact on their INR. Just keep a consistent diet while you're on the course. It really helps the doctors pin down whether the INR spike is from the antibiotic or from a change in what you're eating. Also, don't be afraid to keep a simple log of your dose and any symptoms like those easy bruises mentioned. Having a written record makes those 72-hour check-ins much more productive. We are all in this together to find the safest balance. Just keep communicating with your clinic and you'll get through the course safely.
caesar simpkins
April 25, 2026 AT 21:29Oh man, the thought of a stroke risk just because of one specific antibiotic is absolutely terrifying!
Akshata Kembhavi
April 26, 2026 AT 18:45This is so useful, we have a few family members back home who struggle with their meds and always forget these details.
Tokunbo Elegbe
April 28, 2026 AT 03:06It's so important to be proactive... please, make sure you notify your clinic immediately!!!
aman motamedi
April 29, 2026 AT 03:40The information regarding Rifampin is noted with gratitude.